Summary
DOI: 10.1373/clinchem.2014.229773
A 43-year-old woman with a medical history significant for hypertension, depression, and primary biliary cirrhosis (PBC)3 was admitted to the hospital after outpatient laboratory tests showed hyponatremia. Her complaints on admission included blurry vision, nausea, and significant pruritus.
Student Discussion
Student Discussion Document (pdf)
Midhat S. Farooqi1,2 and Ibrahim A. Hashim1,2*
1Department of Pathology, University of Texas Southwestern Medical Center, Dallas, TX; 2Parkland Health & Hospital System, Dallas, TX.
*Address correspondence to this author at: Department of Pathology, UT Southwestern Medical Center, 5323 Harry Hines Blvd, Dallas, TX. Fax 214-648-8037; E-mail [email protected].
Case Description
A 43-year-old woman with a medical history significant for hypertension, depression, and primary biliary cirrhosis (PBC) was admitted to the hospital after outpatient laboratory tests showed hyponatremia. Her complaints on admission included blurry vision, nausea, and significant pruritus. Her review of systems was otherwise negative. She declared no family history of hypercholesterolemia or premature heart disease. She was taking multiple medications including azathioprine, prednisone, amlodipine, losartan, prochlorperazine, sertraline, trazodone, fenofibrate, ranitidine, hydroxyzine, ursodiol, and cholestyramine. Physical exam was remarkable for scleral icterus and mild jaundice; no xanthomas were noted.
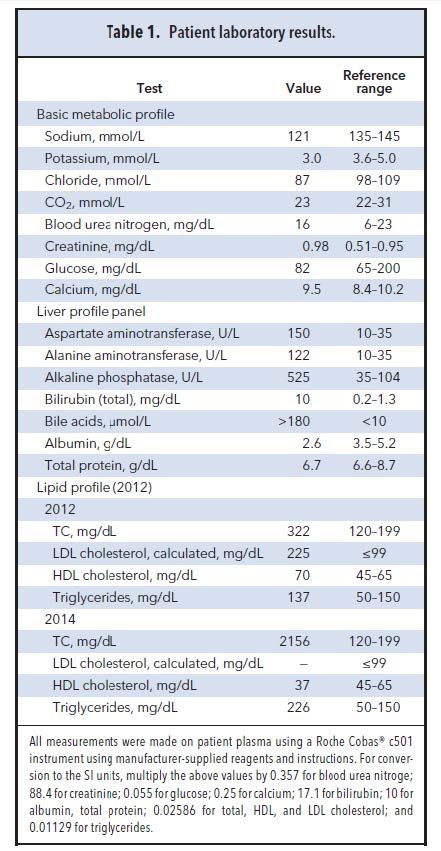
Laboratory studies were performed (Table 1). Once more, the patient was found to have hyponatremia, along with hypokalemia and hypochloremia. Her creatinine was slightly above normal limits but stable compared with past values. A liver profile test panel showed mild increases in transaminases, increased alkaline phosphatase activity, hypoalbuminemia, significant hyperbilirubinemia, and evidence of cholestasis with increased bile acids in the blood.
The patient was started on intravenous fluids (0.9% sodium chloride). Subsequently, a lipid panel was ordered (Table 1). Her most recent total cholesterol (TC) value, measured 1.5 years prior, was 322 mg/dL (8.3 mmol/L). Current testing revealed a markedly increased plasma TC concentration of 2156 mg/dL (55.8 mmol/L). This was the highest TC value ever measured by our laboratory. Furthermore, the sample appearance was clear and not grossly viscous or lipemic. An investigation took place to determine if this was an erroneous result.
Questions to Consider
- What are possible causes of discrepant total cholesterol values?
- What steps can be taken to determine if this was an erroneous result?
- What are the implications for the patient if the results of her lipid panel are accurate?
- What are the mechanisms by which lipemia can interfere with laboratory testing?
Final Publication and Comments
The final published version with discussion and comments from the experts appears
in the August 2015 issue of Clinical Chemistry, approximately 3-4 weeks after the Student Discussion is posted.
Educational Centers
If you are associated with an educational center and would like to receive the cases and
questions 3-4 weeks in advance of publication, please email [email protected].
AACC is pleased to allow free reproduction and distribution of this Clinical Case
Study for personal or classroom discussion use. When photocopying, please make sure
the DOI and copyright notice appear on each copy.
DOI: 10.1373/clinchem.2014.229773
Copyright © 2015 American Association for Clinical Chemistry