 Mike Astion, MD, PhD
Mike Astion, MD, PhD
Editor, Patient Safety Focus
Medical Director, Department of Laboratories
Seattle Children’s Hospital
The benefits of automation have been realized in clinical laboratories more than anywhere else in healthcare. Nonetheless, it is hard to reliably automate everything in the lab, and the manual work that remains is copious and tends to be error-prone. For example, in a lab that processes millions of test requisitions, manual handling of 1% of the requisitions means there are tens of thousands of manual requisitioning events annually, with each posing an opportunity for mistakes.
To cope with these manual processes, it’s important for labs not to become overwhelmed, as there are several reliable steps lab managers can take to mitigate errors—and stress. Labs should focus not only on standardization and accountability, but also on creating a quiet, calm work environment.
One of the best ways to error-proof manual processes is to isolate the work. This means coaching staff to focus only on the task at hand, and not be sucked into multitasking. For example, if the manual work is pipetting, then the pipetting occurs in an interruption-free zone where no other tasks—such as answering the phone—are permitted. To achieve error-free manual work, accuracy rather than speed should be rewarded. Reducing or completely eliminating time constraints can be particularly helpful in this regard.
Smoothing workflow goes hand-in-hand with isolation. In a smooth workflow, staff work at a constant pace, rather than alternating between large peaks and valleys of work. This can be done by having a lead technologist pace the work, or by having those who perform the manual work pull it at a relatively constant pace while receiving feedback that the steady pace is being maintained.
Finally, laboratorians should consider redundant data entry. Also called double entry, redundant data entry involves two separate people entering the data, with data only flowing forward if the two independent entries match. It adds time to data entry, but it dramatically reduces data entry errors when computer interfaces are not an option.
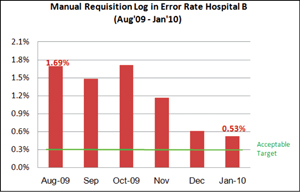
A few years ago, a lab that I worked with tried the interventions in Table 1 to reduce errors in entering the data from manual requisitions into the lab information system. These manual requisitions on paper forms involved tests for which there was no computerized order entry, and they represented a small but significant fraction of the work in the lab. Figure 1 shows the error reduction that we achieved. The lab sustained this improved error rate, which ultimately led to decreased patient harm, improved client satisfaction, and higher staff satisfaction.
Further Reading
- Grimm E, Astion M. Organizing specimen processing for high quality and efficiency: An interview with Linda Nesberg. Clinical Laboratory News 2010;36(10):12–3. Available at: http://www.myadlm.org/publications/cln/2010/October
- Astion M. Smoothing workflow and reducing errors in specimen processing: An interview with Albert Dalbello Jr. and Linda Nesberg. Clinical Laboratory News 2009;35(7):14–5. Available at: http://www.myadlm.org/publications/cln/2009/july/
- Kawado M, Hinotsu S, Matsuyama Y, et al. A comparison of error detection rates between the reading aloud method and the double data entry method. Control Clin Trials 2003;24:560–9.