 An Interview With Sharon M. Geaghan, MD
An Interview With Sharon M. Geaghan, MD
In the July issue of Patient Safety Focus, Dr. Geaghan described the risks associated with capillary blood sampling from a finger-stick puncture, a widely used method in point-of-care glucose testing. Here she expands on that interview, focusing on the heel-stick sampling method, a simple procedure in which a baby's heel is pricked with a lancet and then a small amount of the blood is collected in a narrow-gauge capillary glass tube or on a filter paper. Dr. Geaghan is professor of pathology and pediatrics at Stanford University School of Medicine in Palo Alto, Calif.
Nancy Sasavage, PhD, conducted this interview.
Please describe drawing blood by heel-stick sampling.
The heel-stick method for drawing capillary blood is the most common way to draw newborns' blood. It is used to collect blood for newborn screening tests, usually before the baby leaves the hospital. Heel sticks are the most commonly performed invasive procedure in neonatal intensive care units.
When is the heel-stick method used to draw blood from infants?
That is a frequently asked question. I like to think of this question in terms of developmental milestones. While fingers are the site of choice after infancy, heel sticks are appropriate for most babies, including premature infants, neonates, and even babies 4 to 7 months old. The only caveat is that babies discover other parts of their bodies, such as their feet and toes, as they grow older.
A bandage placed on a baby's heel can pose a safety risk when the child is able to place its feet in its mouth. By 8 to 12 months, babies are pulling themselves up, standing, and preparing to walk or walking; so heel sticks are not recommended at this developmental stage because the heels are bearing weight to varying degrees. Premies may not reach such milestones on the same schedule as full-term babies, so I recommend that parents be questioned about their child's development before performing a heel stick.
What risks are particular to heel sticks?
Improper heel-stick technique can damage the structures of the foot, including the calcaneus bone and soft tissues. In fact, some reports have documented difficulties walking later in life. It is safe to perform a heel stick if the puncture site is limited to the medial and lateral planter aspects of each heel pad, specifically medial to a visual line drawn from the middle of the big toe extending posterior to the heel or lateral to a line drawn from between the fourth and fifth toes and extending posterior to the heel. Repeated punctures, bruising, or erythema limit the available area for punctures, especially in premature infants who may have blood drawn multiple times or very tiny heels.
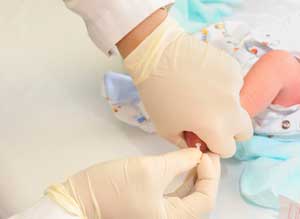
How can heel-stick safety be assessed?
Due to the special technical requirements of this procedure, it is ideal to have experienced staff who perform heel sticks frequently. It is also important to have a program in place to maintain this special skill set. Periodic quality rounds to randomly inspect neonatal heels are a good idea to evaluate staff performance and take corrective actions when necessary.
Editor's Note
The Clinical and Laboratory Standards Institute (CLSI) recently released an updated edition of its standard NBS01-A6, "Blood Collection on Filter Paper for Newborn Screening Programs," which replaces standard LA04-A5. This important document, revised for the first time since 2007, contains a substantial amount of new information on the essentials of correctly collecting a high-quality specimen, handling the specimen after it has been collected, transporting it to the testing facility, and sorting the residual specimen that remains after laboratory testing. For additional information, visit the CLSI website.
Are there other safety risks associated with heel sticks?
Yes, there is also a risk of burning the baby's skin while warming its heel before the blood is drawn. Heel warming is used to increase blood flow in the capillaries. If the heel is to be warmed, using warm water submersion is risky unless you tightly control the temperature.
Chemical heat packs are single-use, and offer a temperature-controlled, safer, but more expensive alternative. Though heel warming is commonly performed to increase blood flow, this protocol is actually based more on theoretical grounds than on any solid evidence that it works. Two studies have claimed that heel warming does not increase blood flow; however, the studies were not blinded (1, 2). It is costly in terms of time and consumables, so a well-designed study to resolve this question would be welcome.
Are finger sticks on infants safe?
Yes, they can be performed with special safety measures. Special lancets less than 1.5-mm thick can be used once heel sticks are no longer an option and after 6 months of age. At that age, distance from the skin surface to bone and cartilage in the middle finger is only 2.5 mm (3).
REFERENCES
- Barker DB, Willets B, Cappendijk VC, et al. Capillary blood sampling: Should the heel be warmed? Arch Dis Child Fetal Neonatal Ed. 1996;74:139–40.
- Janus M, Pinelli J. Comparison of blood sampling using an automated incision device with and without warming the heel. J Perinatol 2002;22:154–8.
- Reiner CB, Meites S, Hayes JR. Optimal sites and depths for skin puncture of infants and children as assessed from anatomical measurements. Clin Chem 1990;36:547–9.