Just 2 days into the new year, UMass Memorial Healthcare in Worcester and Quest Diagnostics inked a final deal that has caught the attention of many in the lab community: a prominent medical center selling off its successful lab outreach business to a national reference lab. The sale appears to contradict a widely accepted narrative of sustained growth for outreach testing at a time when many hospital lab leaders are seeking to boost their business know-how in order to open or expand an outreach testing business. In fact, reports with data as recent as 2011 show growing revenue in this market.
Why sell a highly respected outreach operation just when the market is booming? According to UMass CEO John O'Brien, it's only a matter of time before once healthy profits for hospital outreach labs begin to deflate. The way he sees it, they may have already peaked, and that's why it seemed like a smart move to sell off his outreach business now, O'Brien told CLN. Quest and other big players in the market are betting on O'Brien's being right and have laid out plans for growth that forecast an expanding lab sector that nevertheless becomes increasingly consolidated and competitive. They expect a market ruled by sustained cost pressures that will deflate what they see as a hospital outreach testing bubble.
O'Brien, who helped shape the healthcare reform plan in Massachusetts that inspired President Obama's Affordable Care Act, said he had long anticipated that hospital outreach testing and other areas would struggle in the post-healthcare reform era. He began warning the UMass Medical Center board several years ago that lab outreach and other programs would need to be reevaluated. "We knew that eventually there would be truly crushing pressure on health systems to get their costs down," he said. "Medicare and commercial payers have an imperative to push down prices, and as this moves forward, the big health systems like ours can no longer expect to continue extracting higher prices in the lab and other areas. Quite frankly, those days are gone."
The Race to Acquire Physician Practices
The fate of hospital outreach programs is invariably caught up in larger physician- and hospital-driven trends. And none may be more significant than the rapid pace at which hospitals have acquired physician practices. According to the 2012 edition of the American Hospital Association's Hospital Statistics report, the number of physicians employed by hospitals has grown by 32% since 2000. Now 40% of primary care physicians in the U.S. are employed by hospitals, double the number in 2000. This is a windfall for hospitals because they can drive their physician employees to funnel patients, procedures, and testing back to the hospital system. And so far it's been good news for these hospitals' lab outreach programs, enlarging their market share and increasing per-test revenues.
Laboratorians should expect hospitals to continue pulling in more physicians, with wide effects on the lab market, according to Francisco Velázquez, MD, CEO of PAML, a Spokane, Wash.-based national reference lab co-owned by Providence Health and Services and Catholic Health Initiatives. "I've seen projections that about 75 percent of all physicians will be employed by hospitals within the next three-to-five years, so we know that will be the model we see in healthcare going forward," he said. "This means that the decision-making that used to reside with physician practices or individual practitioners about which labs and other services they will use now belongs to the organization that employs the physician."
So far the trend looks favorable for PAML, Velázquez said, which is already known for creating joint ventures to help hospital outreach labs boost their capabilities. He has witnessed the market become more difficult for many independent labs that now compete for a shrinking pool of autonomous physician practices. "We see more healthcare systems encouraging or even dictating which labs the hospital-owned physician practices can use. Especially in the last 18-to-24 months, we have noticed that a large segment of what used to be free market testing that was open for competition has gone back to the primary ownership institutions or healthcare systems," he said. "We at PAML are fine-tuning our model going forward to accommodate some of these changes and help our hospital partners enhance their position."
At the same time, some in the industry believe that what today is a boon for outreach lab businesses may portend a reversal of their fortunes in the long term. Quest's president and CEO Steve Rusckowski, who in May 2012 left the top post at Philips Healthcare to join the company, warned that the current advantages for hospital labs are real—but temporary. Rusckowski has outlined a strategy for Quest that runs the gamut from providing esoteric testing services and lab management to stepping in to partner with hospitals when, under pressure from payers, they run into trouble. Quest already has six joint ventures with hospitals across the country and plans to forge more of these agreements, in addition to courting hospitals that wish to outsource part or all of their lab operations, or sell off segments of the business such as UMass has done.
"When you look at reimbursement on the commercial side, in many cases there is a premium for services provided by a hospital versus an independent organization like ourselves," Rusckowski said. "Certainly, payers are seeing these differences in price and are asking the question, why should we do the same work in a more expensive place? As hospitals continue to absorb physicians, payers will increasingly realize how large this cost is and will begin to narrow their networks for lab services. At the same time, hospital CEOs also realize that high prices are not sustainable, and will be looking for strategic partnership opportunities with a world-class supplier like ourselves."
LabCorp also sees opportunity in a changing lab market. Its subsidiary, Beacon Laboratory Benefits Solutions, is seeking to negotiate between networks of hospital labs and independent labs on the one side, and health plans on the other, with services such as physician decision support, billing, and analytics. As an intermediary, Beacon becomes the gatekeeper and negotiator, similar to pharmacy benefit management companies.
A Snapshot of the U.S. Lab Market
Total U.S. Lab Market—$72 Billion
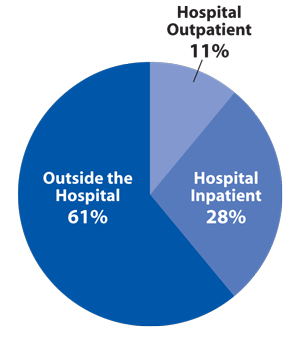 Outside the Hospital Lab Segment—$44 Billion
Outside the Hospital Lab Segment—$44 Billion
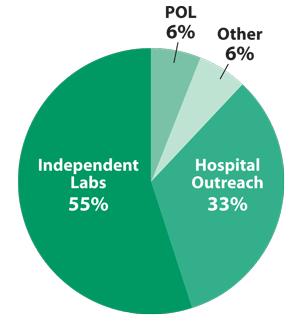 Independent Lab Segment—$24 Billion
Independent Lab Segment—$24 Billion
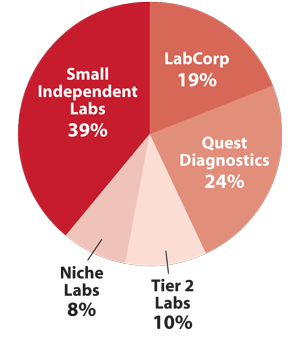
A Spotlight on Test Prices
How far hospitals can come down in price—or in fact, if they ought to—in order to directly compete with independent commercial labs is a matter of contention. But no one questions that payers and consumers are taking notice.
In the past, noted UMass's O'Brien, hospitals could cope with declining reimbursement from Medicare and other government payers by shifting some of their costs to commercial payers and charging them more than Medicare. Now, commercial insurers are arriving at an inflection point, where premium increases are capped but costs continue their curve upward. As a result, payers have redoubled their efforts to extract savings from providers. "I think a lot of health system leaders are thinking that they'll be able to wait this thing out," O'Brien said. "But the reality is the train has already left the station. If we want to sustain our operations, we're going to have to look to people in the past who have been our competitors and make them our partners."
Using new authority under the Affordable Care Act, several states have taken action recently to force insurers to cut their premium increases. In New Mexico, the state insurance division denied a request from Presbyterian Healthcare for a 9.7% rate hike, lowering it to 4.7%. And in Connecticut, the state stopped Anthem Blue Cross Blue Shield, the state's largest insurer, from hiking rates by a proposed 12.9%, instead limiting it to a 3.9% increase.
Financial analysts that keep tabs on publicly traded firms like Quest and LabCorp have recently advised investors that the large commercial labs could have an advantage as payers aggressively seek low-cost providers. According to Kevin Ellich, a senior research analyst at the investment bank Piper Jaffray, hospital acquisitions of physicians' practices have hurt independent labs in recent years. However, he emphasized that he believes hospitals are driving up costs compared to independent labs.
In an October 2012 research report for investors, Ellich noted that "the near-term environment remains somewhat challenging" for commercial independent labs like Quest and LabCorp due to slow growth and reimbursement challenges; however, these companies "could benefit from a longer-term paradigm shift as lab customers (physicians) and patients seek low-cost providers."
In his report, Ellich offered his own recent test results as an example. After receiving a bill from what he learned was a hospital outreach lab, he contacted his insurer to compare prices. The insurer could only offer comparison prices for Quest, but Ellich said he believed LabCorp would have been similar. Ellich learned that the total charge from the outreach lab was $650, while the cost at Quest would have been $145–348% lower. Ellich emphasized that this meant higher out-of-pocket costs for him. His 20% coinsurance was $80.82 for the hospital outreach lab, compared to $29 had he gone to Quest. Ellich isn't the first to observe that hospital-based testing costs more, at least on a price-per-test basis. The bigger picture, he told CLN, is that cost sharing is on the rise for commercial health plans, and out-of-pocket spending will hit consumers hard as coinsurance and deductibles creep higher.
Furthermore, for physicians who do have a choice about where to refer patients for lab testing, bundled payment models favored by Medicare and commercial insurers would incentivize physicians to steer lab testing toward the lowest-cost provider. "Right now, the physician is an apathetic customer who doesn't really care where testing is performed or how much it costs," Ellich said. "But as we move toward payment models with bundled or capitated payment, that will change. If my physician gets a capitated payment that includes some of the lab work, he's definitely going to send me to Quest or LabCorp rather than a hospital lab that costs twice as much."
Quest's Rusckowski stressed that he believes healthcare reform will be a net positive for the lab market, beginning in 2014 when some 30 million more people gain health insurance. He expects the lab market to grow at a rate of about 4% per year. However, how the additional volume and dollars will move through the healthcare system will change. "We are going to spend more money on healthcare for the foreseeable future in the United States, and that money has to go someplace," Rusckowski said. "But we need to think this through. Yes, there will be more volume; however, on a per-test volume basis we will see less money as we move toward a capitated payment system for episodes of care. The lab industry needs to consider how we build our business around that."
Health Plans Gain Leverage as Costs Climb
As hospitals have shored up their position as the center of the healthcare universe, commercial payers have learned to leverage their own power in surprising ways. With employers desperate to keep down the cost of their health plans, insurers have gained clout to prod, pressure, or exclude labs that ask for better pricing. Some insurers, like Aetna, send letters to patients urging them to avoid hospital labs in favor of national reference labs, with charts that show high out-of-pocket costs for hospital labs.
Insurers are also exerting influence by contacting self-insured employers with comparative cost data, giving the employers incentive to steer employees directly toward the lowest cost labs, explained Michael Snyder, who previously worked at both LabCorp and UnitedHealthcare and is now the principal of Clinical Lab Business Solutions, a laboratory management consulting firm. "Employers are keeping their fingers on the health plans to keep down premium costs. So with the employers on their side, health plans have aggressively sought deals with the Quests and the LabCorps of the world for very, very low costs," Snyder said. "The reason they can do this is that Quest and LabCorp are very efficient. Right now, much of the pricing with the major health plans is somewhere around 50 percent of Medicare, which is just crazy. It's the only health service in the U.S. that actually sells for less than Medicare on the private side."
More recently, insurers have evolved their strategies and escalated from making super low-cost in-network deals to outright exclusion of labs if they see a higher per-test price. Snyder offered the example of one of his clients, a large health system in the South that asked for help with its lab outreach. "In their case, not only was the insurer steering away from them, but some of the larger employer groups were actually excluding them with respect to the lab," Snyder said. "So even if the hospital had a facility contract with the insurer—yes, they could get paid for inpatient, for emergency care, for ambulatory surgery—but for outreach testing, that payment would be denied altogether. This is an example of how health plans are gaining traction quite quickly, so it's really incumbent on hospital labs to do some things differently than they did in the past."
New Strategies for Outreach
Few hospital labs are likely to make it in the post-reform market if they decide to go it alone. However, if they are willing to change, Snyder believes hospital labs can still succeed by collaborating with others. First, hospitals can bring down their prices, though the prospect is painful. "Labs have got to be able to sell this to hospital executives and make them understand that, yes, they'll take in a little less money, but there remains an opportunity to hold onto the outreach business and make it a value proposition for health plans," Snyder said.
One way individual outreach labs can make themselves more attractive to health plans is to band together in joint venture or other collaborative models. "Working together makes hospital labs easier to work with for the insurers," Snyder said. "Right now, they see a fragmented and inefficient market." For example, more than 100 hospital labs in Michigan worked together under the umbrella Joint Venture Hospital Laboratories and won a Blue Cross Blue Shield contract for most of the state.
The hospital also has a secret weapon in competing with independent labs that is right under its nose: inpatient testing. Traditionally, hospitals saw the cost of inpatient testing as a drag on their business, which in turn drove outreach in an effort to use the lab's excess capacity. From a different perspective, though, Snyder says that hospital labs should showcase their management of inpatient testing under the flat payments of diagnosis related groups (DRGs) as proof that they are the true utilization management experts.
"The labs are already experts at controlling utilization in the hospital, so if they can demonstrate that they will translate that to the outpatient side as well, they've got something of great value to the health plan," Snyder said. "They're also already part of the continuum of care—they have both the inpatient and outpatient record. If the hospital can show how their lab contributes to care management, then they're helping the health plan save on the 97 percent of spending that occurs outside the lab. That's very powerful."
PAML's Velázquez agreed. "Can hospital labs be as competitive as large, national independent labs on a cost-per-test basis? Maybe. But when we go into a market and work with a healthcare system, we're not looking for a price war, because commoditizing lab medicine is not a very good strategy," he said. "We are competitive because of the overall value that we bring that goes far beyond the price of that test. When we show the lab is part of better outcomes, of really controlling risk for disease in a community, this is where we can make a difference."
PAML—known for its successful reference lab and joint ventures with hospital labs—in 2013 will launch additional services beyond its current suite of utilization management, billing, logistics, and other offerings for hospital labs. The new service is still under wraps, but Velázquez hinted it involves so-called "big data": information management solutions that integrate lab data with other patient information.
To be sure, Quest, LabCorp, and other independent labs are leveraging their size and capital to invest in utilization management and IT solutions as they court health plans and hospital systems. Whether hospital labs partner with an independent lab or join forces with other hospitals, they'll need to update their strategy, Snyder emphasized. "What labs need to do is take the next step. Right now, we often just throw results over the wall, whereas if we take that continuum of data, transform that data into knowledge, and that knowledge into actionable intelligence, then we have a new product," he said. "But it's a horse race now. The hard thing is convincing folks that hospital labs should do this, rather than just scooping up those results and letting someone else do it for them."