Medicare and other payers are increasingly targeting overutilization as a way to curb healthcare costs. This year, the Centers for Medicare and Medicaid Services (CMS) launches two major programs from the Affordable Care Act designed not only to reduce costs but also to improve quality—accountable care organizations and the bundled payment initiative. To share in the financial savings from these programs, providers must demonstrate that they meet cost and quality benchmarks.
Forward thinking laboratorians are taking advantage of this environment to make the lab part of the solution, positioning themselves as utilization experts who can improve the quality and efficiency of care. To varying degrees, they are following the model that pharmacists created decades ago when they worked with their physician colleagues to form pharmacy and therapeutics committees. Some laboratorians are even managing their test menu as a lab formulary, contributing their expertise to help control who can order tests and when.
According to Paul Levy, MD, chair of the laboratory diagnostics committee for the University of Rochester Medical Center (URMC), the concept of the lab formulary at URMC originated with a concern over the escalating cost of send-out testing, but has become much more than that. URMC is one of a small but burgeoning number of institutions with a published, tiered formulary for send-out testing managed by a special committee. "The realities of reference lab tests in particular, and especially the growing number of genetic tests, are such that many clinicians aren't quite sure what they're ordering and how that result might influence patient care," said Levy. "So the laboratory diagnostics committee's real charge, even though it started with concerns about costs, was to improve alignment between medical necessity and the tests themselves." Levy is also the Charles A. Dewey Professor and Chair of the department of medicine at the University of Rochester School of Medicine and Dentistry.
The Test Menu as Formulary
Although utilization management is not new to labs, not many have taken the step of limiting access to certain tests on their menus. Even fewer have established an official lab formulary and published it as such. As one of these, URMC stuck closely to the pharmacy model, clearly stating that off-formulary tests would no longer be available through URMC labs. Just like a drug formulary, URMC set up a three-tier system for all reference testing and published it online last year.
Tier 1 tests are available to all providers, while tests in tier 2 are restricted to subspecialists. Only board-certified, subspecialty-trained physicians holding faculty appointments at URMC or staff privileges at two affiliated hospitals may order tests on this list. The idea is that certain tests require a high level of expertise in a specialty area and other clinicians should not normally be ordering them, Levy explained. "If there is a tier one test that might have a little bit of a neurology flavor to it, as a pulmonary specialist, I could still order that test if it's on tier one," Levy said. "With more esoteric specialized tests that neurologists felt required specialty skills, we placed those in tier two." The laboratory diagnostics committee manages the formulary, but also seeks help from subcommittees of specialists for tier 2 tests. The committee includes pathologists as well as specialists from neurology, oncology, and pediatrics.
Off-formulary, or tier 3, tests are not impossible to order, but require a review from the laboratory diagnostics committee. Clinicians can choose a one-time authorization request for an urgent medical need or submit a form requesting that a test be permanently added to the formulary. In the latter case, the clinician must explain in writing how the test would influence clinical management, treatment plans, and patient care. Levy described the process as a "rigorous medical necessity appeal."
Brigham and Women's Hospital in Boston also publishes a reference lab formulary online, but splits the third, off-formulary tier into two categories: unauthorized, and undefined. Selected by the hospital's advanced laboratory diagnostics review committee, unauthorized tests are strictly off limits, while tests in the undefined—or, essentially, unlisted—category may be performed in an emergency or in the case of an irreplaceable specimen. Similar to URMC, if physicians want to order non-emergency tests that are undefined, they must submit a written proposal for review by the committee.
Other labs have stepped up the management of their test menus and put some restrictions in place, but not published an official formulary per se. At Massachusetts General Hospital (MGH) in Boston, most utilization management efforts rely on computerized physician order entry (CPOE) and electronic health records (EHR), in tandem with collaborative work on test ordering guidelines and education for targeted areas. A group from MGH last year described their decade-long quest to fine-tune a variety of utilization management strategies (Am J Clin Pathol 2011;135:108–118).
Anand Dighe, a coauthor of the paper and director of the core lab at MGH, explained how MGH combines electronic-based barriers to certain tests as well as lots of face time with specialty groups for problem areas. "The main way that we implement our formulary is by not having tests on the menu that shouldn't be there," he said. "We've also cut down the menu on our inpatient order entry system, which is principally used by interns, residents, and fellows. We really don't want to expose them to all of the possible send-out genetic tests." Dighe is also an assistant professor of pathology at Harvard Medical School.
Similar to URMC, some tests at MGH cannot be ordered easily through the CPOE by non-specialists. "We don't make it impossible to order a genetic test; we just make it slightly more onerous and require a conversation with a pathologist before it's sent out," said Dighe. "We have a lot of tests on our borderline list, where we don't feel they're needed for clinical care, but they're still being sent out. And those are the ones that are monitored closely by our clinical laboratory advisory committee."
The MGH clinical laboratory advisory committee is made up of pathologists and others from across the hospital. Dighe stressed that the committee reports directly to the hospital's medical policy committee, which includes top administrators and physician leaders. "If you're going to take a formulary approach, it has to have some legitimacy and staying power," Dighe said. "By having a formulary endorsed by a group that reports to the medical policy committee, it gives it more authority."
Despite the need to curb unnecessary testing, laboratorians would do well to remember that the lab is still different from pharmacy in several important ways, noted Michael Laposata, MD, PhD, executive vice chair of pathology and director of the division of laboratory medicine and clinical laboratories at Vanderbilt University Medical Center in Nashville. "In pharmacy, there is a lot of evidence of head-to-head drug testing where you can point to a study and say, ‘there it is, that's the answer.' But often lab tests are not that simple," Laposata said. "There is far less of an established database on the indication for a lab test than the indication for a drug." Laposata is also the Edward and Nancy Fody Professor of Medicine and Pathology at Vanderbilt University Medical Center.
Laposata, a well-known expert on consultative lab medicine, is an advocate for educating clinicians about appropriate utilization of lab testing. But he also encourages labs to keep the patient in mind when considering limiting access to testing. He offered the example of a patient with a rare genetic mutation. "It could be that the only person who will care about the rare mutation is the person who has it. Think about cystic fibrosis. Do you think the person's physician tracks the clinical significance of all 1,800 mutations?"
Laposata also noted that often laboratorians will argue that if a frequently ordered test is almost always negative, it's not really adding value. Clinicians frequently use a negative test to narrow the differential diagnosis. "That argument by the laboratorian, who tries to be analytical and says they ordered it so many times and it was never positive, doesn't mean anything to the clinician," he said.
Though others at Vanderbilt have suggested the lab publish a formulary to help control rising send-out costs, for now, Laposata plans to focus on closely monitoring utilization trends for problems, as well as training laboratorians to communicate more effectively with clinicians. Vanderbilt is in the early stages of establishing a lab utilization committee for this purpose. "It will have some flavor of a lab formulary committee, but no one is going to throw away anybody's cerebral spinal fluid, even if it costs $5,000 to perform the test," Laposata said.
Working with Clinicians
With all test utilization efforts, at some point the project comes down to the lab's relationship with ordering clinicians, whether mediated by a CPOE, the telephone, or the intimacy of a face-to-face conference.
Dighe emphasized that MGH has taken a measured approach to restricting access to tests, preferring to work with physicians on practice standards for tests rather than perfunctorily trimming the menu. "We've picked our battles here," Dighe said. "We have not gone with broad brushstrokes and said we're going to put limits for every single person in the system." When Dighe and his colleagues analyzed their spending on send-out tests, they found that a third of the expense was coming from just several dozen providers—some $3 million worth. They also found that many of these individuals worked in the same groups. As a result, instead of making across-the-board changes to the menu, lab leaders attended the group's monthly meetings and presented data on lab testing.
In some cases, these meetings led to new practice standards that helped providers manage utilization on their own—and with great success. After working with the pediatric genetics group, MGH saved more than $400,000 with more appropriate lab testing. "These are all experts in their field. If you just yank the test off the menu, in addition to the fact that is does not promote collegiality and collaboration—you are missing an opportunity: your providers more often are more knowledgeable about the test than you are," Dighe said. "We don't want primary care providers ordering $10,000 genetic test panels, but on the other hand, we do want to have a discussion with our neurologists and our geneticists about when it's appropriate to order these tests."
At the Veterans Affairs (VA) Connecticut Health System in New Haven, the lab is also taking an active role in lab utilization, starting with the reference lab menu. The VA uses a financial cutoff for all send-out testing, after which the ordering provider must consult with the lab. A lab technologist pulls an electronic record of all the send-out tests costing more than $35 and passes along these requests to a team of attending pathologists and laboratory medicine residents. "The lab reviews these orders and determines whether the test is appropriate, or if there is potentially another in-house, less costly, or even better test for that patient," explained Christopher Tormey, MD, assistant professor of laboratory medicine at Yale University School of Medicine and a clinical pathologist at the VA Connecticut Healthcare System. "They then communicate with the clinician who ordered the test and discuss potential ordering options. At that point, they either agree to cancel the test, change the order, or in many cases the test that was requested is appropriate and it's ultimately sent out." According to Tormey, this strategy helps to control costs, assure clinical utility, and keeps the lab apprised of new trends in clinician ordering.
Often, the lab doesn't have to lean too hard on clinicians when their review concludes that a test is unnecessary. "We often just ask the clinician how the test will influence patient management. And many times when they're confronted with that question, they don't have a very good answer," Tormey said. "I think there is this general thought among some clinicians that it's just good to know this information, but when specifically asked how it'll change patient management, it can turn out to be purely an academic pursuit and there is nothing to be gained."
In addition, the VA Connecticut has worked on algorithms for certain problem areas of utilization, a kind of reverse-reflex system that acts as an electronic gatekeeper. These algorithms depend on a highly functional EHR that contains all the patient's lab data. Rather than requiring a conversation with the lab in all cases, the algorithm will allow the test to be sent out if certain clinical conditions are met (See Box, below).
Algorithms Help Assure Appropriate Testing
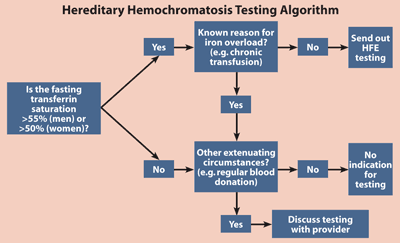
One approach to utilization management that’s been particularly successful at the Veterans Affairs Connecticut Health System in New Haven has been targeting expensive send-out tests with algorithms that assure each order is appropriate. Rather than require approval from the lab in all cases, the algorithm will allow the test to be sent out if certain clinical conditions are met. So far, the VA has only tried this approach with a handful of tests, including methylmalonic acid, hepatitis B DNA polymerase chain reaction, IL28B single nucleotide polymorphism, and hereditary hemochromatosis. Along with other strategies, the algorithms have saved upwards of $100,000 a year, according to Christopher Tormey, MD, assistant professor of laboratory medicine at Yale University School of Medicine and a clinical pathologist at the VA Connecticut Healthcare System. “For our facility, that’s a significant portion of our send-out budget. So we think that this is a meaningful cost-savings, and as we roll out other initiatives, like targeting high-volume tests and trying to knock down unnecessary repeat testing, we think those numbers will only increase,” Tormey said. “We think it’s better for the patients as well, because sometimes physicians make decisions based on tests that are really not appropriate.”
Tormey said he sees the potential in having a true formulary that would completely restrict certain tests. "This would be particularly useful in the cases where the lab and the clinician are at odds," he said. "There are certainly situations where our model fails because a clinician absolutely insists on ordering a test of questionable utility," he said. "I think the formulary approach is a way to have the administration really support you in declining something that by all evidence and expert opinion is not necessary for that patient."
David Bernard, MD, PhD, medical director of clinical pathology at The Methodist Hospital in Houston, also emphasized a hybrid approach—influencing test selection via technology, but also spending time with providers one-on-one. Except for specialists that the lab trusts to order the more expensive, esoteric tests, a cost limit for send-out tests requires the provider to contact the lab. "In these cases we use the ‘telephone net' and the ‘sneaker net' to talk to the ordering physicians," Bernard explained. "We ask them, ‘why are you doing this test, and what are you going to do in this episode of care for this patient with this result.'" At The Methodist Hospital, Bernard is also medical director of referral testing and laboratory medicine IT, as well as the chief medical information officer. He is a senior member of The Methodist Hospital Research Institute, and an associate professor of clinical pathology and laboratory medicine at Weill Cornell Medical College of Cornell University.
It helps that, similar to MGH and the VA Connecticut, the Methodist Hospital is on the cutting edge when it comes to CPOE and EHR technologies. In what seems like light-years away from traditional lab requisitions, Bernard has focused on perfecting the order sets in the hospital's EHR. These are the lab test selections on the computer offered to clinicians based on patient symptoms or episodes, or on admission with certain diagnosis codes.
Bernard collaborates with clinicians at the hospital to develop these mini lab menus, making sure only appropriate tests show up on the screen for each scenario. Every time an order set is developed, the hospital's laboratory performance improvement committee meets to agree on which testing options should be included. "We still allow the doc to go into the full test catalogue if they want, but make it harder for them to do so,t and they are less likely to do it unless they really go looking for it," Bernard commented. "This is one tool that has the potential for a big impact across the system."
What's Next
Ultimately, each lab will need a unique combination of strategies that fits their organization. However, most of the successful approaches that laboratorians are using for lab utilization management seem to have several elements in common, one of which is an innovative use of information technology (IT). Such efforts may be arriving at the right time, as this is the second year of CMS's EHR incentive program, whereby providers can receive up to $44,000 over 5 years by demonstrating at least basic EHR use. In fact, to receive the maximum EHR incentive payment, providers must begin participating by the end of 2012.
"I think most of the limitations on setting up these kinds of filters or formularies will depend on the robustness of your electronic system," Tormey said. "Ideally, we'd be stopping all the inappropriate tests before they're ordered with clinical decision support, by giving the clinicians data about the test itself or about the patient. In some ways this is a justification for a top-notch EHR."
As EHRs become more advanced and more common, other changes technological advances will bring changes to the lab as well, noted Dighe. "I think this is a unique time for these genetic tests. We all know that the prices for these tests are going to plummet. If you can potentially sequence an entire human genome for $100 in five years, no one is going to pay $10,000 for a genetic test like they do currently," Dighe said. "This is even more of a reason to leverage the lab's expertise when the organization is deciding what tests are on the menu, what technologies are used, and how those results are interpreted.
Examples of Lab Formularies
These two institutions make their formularies available online.
University of Rochester Medical Center
URMC website
Brigham and Women's Hospital
BWH website